Why High-Performing Women with ADHD Traits Suddenly Struggle with Focus in Mid-Career
Mar 19, 2026Many high-performing women reach their 40s and begin to notice something unsettling.
Their focus changes.
Their mental clarity fluctuates.
Tasks that once felt effortless suddenly require significantly more effort.
For women who have built careers on being reliable, capable and cognitively sharp, this can feel deeply disorienting.
If this is happening to you, it's important for you to know that you are not losing your ability.
What you may be experiencing is the intersection of ADHD traits, hormonal changes, and cognitive load - a combination that is increasingly recognised in emerging research but still widely misunderstood in professional contexts (Brinton et al., 2015; Weber et al., 2013).
The Overlooked Link Between ADHD and Hormones
ADHD is often underdiagnosed in women, particularly those who are high-functioning and high-achieving (Quinn, 2005; Hinshaw et al., 2022).
Rather than presenting as hyperactivity, ADHD traits in women often include:
-
difficulty sustaining attention
-
challenges with task initiation
-
overwhelm when managing multiple demands
-
reliance on external systems to stay organised
-
cycles of hyperfocus followed by exhaustion
Many women develop compensatory strategies, (often referred to as masking) that allow them to perform at a high level for years (Quinn, 2005).
However, these strategies often depend on relatively stable dopaminergic function, which is influenced by hormonal activity.
Oestrogen, Dopamine and Executive Function
Oestrogen plays a critical role in modulating neurotransmitter systems, particularly dopamine, which is central to executive skills, such as, focus, emotional regulation, planning and time management (Jacobs & D’Esposito, 2011).
Dopamine activity in the prefrontal cortex underpins executive functioning, often impacting:
-
working memory
-
cognitive flexibility
-
decision-making
-
sustained attention
Research has shown that oestrogen enhances dopaminergic activity in these brain regions, improving cognitive performance (Jacobs & D’Esposito, 2011; Hampson, 2018).
During perimenopause, however, oestrogen levels fluctuate unpredictably and gradually decline.
This transition is associated with measurable changes in:
-
attention
-
memory
-
processing speed
(Brinton et al., 2015; Weber et al., 2013)
As oestrogen declines, dopamine regulation becomes less stable, which can directly affect executive functioning.
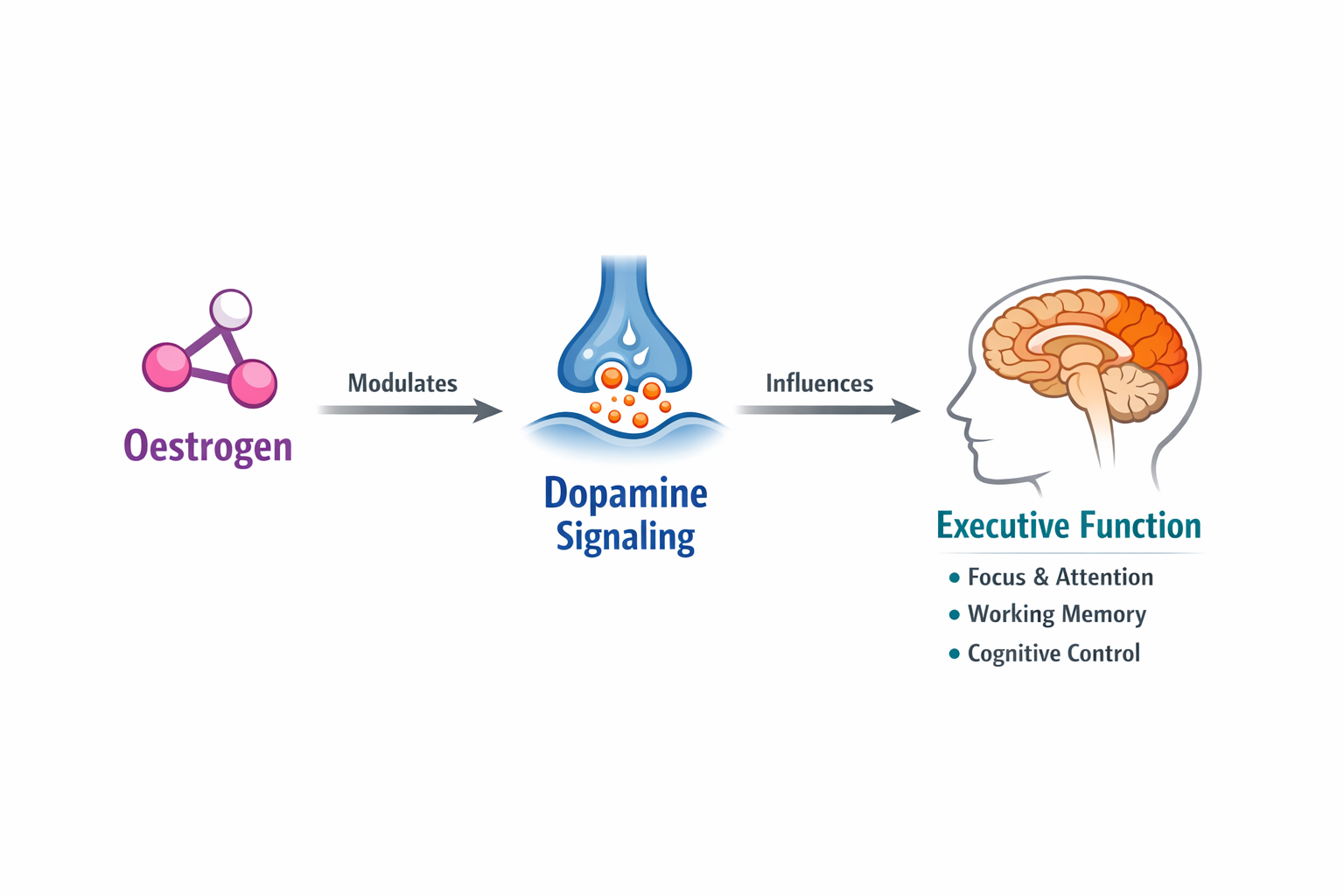 Oestrogen modulates dopamine activity in the prefrontal cortex, a brain region responsible for executive function, attention and working memory (Jacobs & D’Esposito, 2011). Fluctuating oestrogen levels during perimenopause can therefore influence cognitive performance.
Oestrogen modulates dopamine activity in the prefrontal cortex, a brain region responsible for executive function, attention and working memory (Jacobs & D’Esposito, 2011). Fluctuating oestrogen levels during perimenopause can therefore influence cognitive performance.
When Perimenopause Mimics ADHD
For women without a prior ADHD diagnosis, the cognitive effects of perimenopause can closely resemble ADHD-like symptoms.
Common experiences include:
-
difficulty maintaining focus in meetings
-
losing track of conversations
-
increased forgetfulness
-
difficulty prioritising tasks
-
heightened mental overload
These changes are consistent with research describing perimenopause as a neurological transition state, characterised by shifts in brain metabolism and cognitive function (Brinton et al., 2015).
Importantly, these symptoms do not indicate reduced intelligence or capability, but rather reflect changes in neuroendocrine functioning.
When ADHD Already Exists
For women with ADHD, hormonal changes can significantly exacerbate symptoms.
ADHD is strongly linked to dysregulation of dopamine pathways (Del Campo et al., 2011). When oestrogen levels decline, the modulation of these pathways is reduced, which often leads to intensifying ADHD-related challenges.
Studies have shown that women report worsening ADHD symptoms during periods of hormonal fluctuation, including the menstrual cycle, postpartum period, and perimenopause (Epperson et al., 2015; Quinn, 2005).
In perimenopause, this can lead to:
-
reduced effectiveness of coping strategies
-
increased difficulty with attention and organisation
-
emotional dysregulation
-
inability to maintain previous levels of performance
As a result, many women find that they can no longer “mask” their symptoms in the same way.
The Problem with Traditional Productivity Models
Most workplace expectations are built on the assumption that cognitive performance is stable and consistent over time.
However, both neuroscience and endocrinology suggest otherwise.
Cognitive performance is influenced by:
-
neurochemistry
-
hormonal fluctuations
-
stress levels
-
cognitive load
(McEwen & Morrison, 2013)
For women experiencing hormonal transitions, this means that productivity may follow a more rhythmic pattern rather than a linear one.
Ignoring this reality can contribute to cycles of:
overwork → cognitive fatigue → reduced performance → self-criticism → increased effort→ overwhelm
A More Effective Approach: Reclaiming Your Rhythm
Rather than attempting to maintain constant output, a more effective approach is to align with how the brain and body are functioning, in each season of life.
Three key elements support this shift:
1. Clarity
Understanding the interaction between hormones, dopamine and cognitive function reduces self-blame and enables more effective adaptation.
👉 Read more: ADHD masking in high performing teams
2. Nervous System Regulation
Chronic stress impairs prefrontal cortex function, further reducing executive capacity (McEwen & Morrison, 2013).
Regulating the nervous system supports:
-
improved focus
-
better decision-making
-
increased cognitive resilience
👉 Read more: Perfectionism and Burnout
3. Supportive Structure
Flexible systems that align with energy and attention patterns are more effective than rigid productivity models, particularly for individuals with ADHD traits.
You Are Not Losing Your Edge
A key takeaway from both research and practice is this:
Cognitive changes during midlife are not a loss of ability.
They are a reflection of changing biological conditions.
When these changes are understood, it becomes possible to adapt - and to continue performing at a high level in a more sustainable way.
Sounding All Too Familiar?
If you have been finding this all too familiar, you may be at a point where traditional strategies are no longer effective.
This is exactly why I created Unstuck: Reclaim Your Rhythm™ - a 6-week group coaching program designed for high-performing women navigating:
-
cognitive overwhelm
-
fluctuating focus
-
changing energy patterns
The program focuses on:
-
understanding your cognitive and hormonal patterns
-
resetting your nervous system
-
building sustainable, personalised structures
Commonly Asked Questions
Can perimenopause affect ADHD symptoms?
Yes. Hormonal fluctuations, particularly declines in oestrogen, can affect dopamine regulation and exacerbate ADHD symptoms (Epperson et al., 2015).
Why does my focus feel worse in my 40s?
Changes in oestrogen levels during perimenopause can impact brain regions responsible for attention and executive function (Brinton et al., 2015).
Is this ADHD or hormones?
It can be either - or both. Hormonal changes can mimic ADHD symptoms or intensify existing traits.
Can these cognitive changes be managed?
Yes. Understanding the underlying mechanisms and adapting strategies can significantly improve focus and performance.
References
Brinton, R. D., Yao, J., Yin, F., Mack, W. J., & Cadenas, E. (2015). Perimenopause as a neurological transition state. Frontiers in Neuroendocrinology, 36, 1–17.
Del Campo, N., Chamberlain, S. R., Sahakian, B. J., & Robbins, T. W. (2011). The roles of dopamine and noradrenaline in ADHD. Biological Psychiatry, 69(12), e145–e157.
Epperson, C. N., et al. (2015). ADHD symptom changes across the menopausal transition. Maturitas, 81(2), 284–290.
Hampson, E. (2018). Estrogen-related variations in human spatial and articulatory-motor skills. Psychoneuroendocrinology, 98, 14–23.
Hinshaw, S. P., Nguyen, P. T., O’Grady, S. M., & Rosenthal, E. A. (2022). Annual Research Review: Attention-deficit/hyperactivity disorder in girls and women. Journal of Child Psychology and Psychiatry, 63(4), 484–510.
Jacobs, E. G., & D’Esposito, M. (2011). Estrogen shapes dopamine-dependent cognitive processes. Nature Reviews Neuroscience, 12(12), 698–706.
McEwen, B. S., & Morrison, J. H. (2013). The brain on stress: vulnerability and plasticity. Neuron, 79(1), 16–29.
Quinn, P. O. (2005). Treating adolescent girls and women with ADHD. Journal of Clinical Psychology, 61(5), 579–587.
Weber, M. T., Rubin, L. H., & Maki, P. M. (2013). Cognition in perimenopause. Menopause, 20(5), 511–517.
Want to learn more?
Sign up and share your interests with us.
We want to share current information that is meaningful to you.
We hate SPAM. We will never sell your information, for any reason.
